PMMC Newsroom

PMMC Deploys New Client Survey
April 8, 2024
Beginning in April through the second quarter of 2024, PMMC is set to roll out a quick two-question survey in its applications. This new initiative aims to harness valuable client insights to enhance product features and assist users in bolstering their financial outcomes. With this new step towards engaging users in the development process, PMMC reiterates its commitment to client satisfaction and operational excellence.

PMMC Announces Executive Edge Series
March 26, 2024
PMMC announced an educational series set to take place in 2024 starting in April. This is an exclusive leadership series tailored for the enterprising minds of healthcare. Our series promises insightful sessions where executives like you gain access to the expertise of a range of experts who have walked in your shoes and reaped the rewards of the strategies you will uncover. David Zerfoss, Master Chair of Vistage Worldwide will join the PMMC Team as the first of 4 experts.

Scott Soucy, Catholic Medical Center Recognized as PMMC Star of the Month
December 18, 2023
PMMC would like to congratulate Scott Soucy, Director, Managed Care Contracting, from Catholic Medical Center as PMMC’s Star of the Month! Scott is recognized as a client that goes above and beyond in his role. He demonstrates the core values that make a true impact in the lives Scott touches.

Newly Announced Chief Sales Officer Brings Extensive Healthcare Experience
October 16, 2023
Gil Sheek joins PMMC as Chief Sales Officer following a decorated career at Amerisource Bergen bringing extensive healthcare knowledge and experience to PMMC clients.

PMMC Gains HFMA Peer Review for over 10 Years
October 3, 2023
The Healthcare Financial Management Association (HFMA) announced that, following rigorous review, PMMC has once again achieved the “Peer Reviewed by HFMA®” designation for its contract management (Contract PRO) and its patient estimation solution (Estimator PRO) products within its revenue cycle management platform.

Intermountain Healthcare Partners with PMMC for Digital Price Transparency Strategy
September 23, 2021
Intermountain Healthcare, Utah's largest healthcare provider, selected PMMC as its partner to improve the patient experience with a digital price transparency strategy.

Southwestern Health Resources Selects PMMC for Revenue Cycle Contract Modeling
May 25, 2021
PMMC was selected by Southwestern Health Resources, a 29 hospital system in Texas, as its strategic partner for revenue cycle contract modeling.

PMMC Earns HFMA Peer Review Designation for Revenue Cycle Solutions
November 5, 2020
PMMC renewed the HFMA Peer Review Designation for its contract management and patient estimation solutions within its revenue cycle management platform.
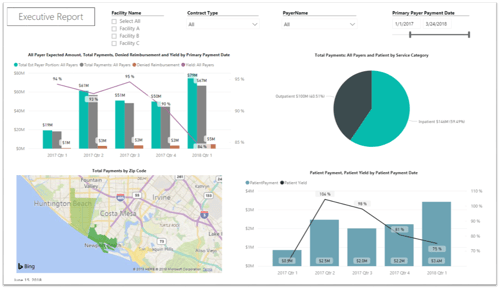
PMMC Launches Game-Changing Analytics Platform for Healthcare Revenue Cycle
June 25, 2018
PMMC launched a game-changing revenue cycle analytics platform at the HFMA Annual Conference that will change the way healthcare financial executives evaluate payer contract performance and drive revenue strategies at their organizations.

Mercy Health Selects PMMC as Strategic Partner for Contract Management and Modeling
February 19, 2018
PMMC was selected by Mercy Health, Ohio's largest health system, as its strategic partner for contract management.
.jpeg?width=900&name=AdobeStock%20(tablet,%20lap%20top,%20business%20peopl).jpeg)
PMMC's Bundling Analytics Help Healthcare Providers Navigate New BPCI Advanced Model
January 22, 2018
PMMC is equipping healthcare providers with the necessary bundled episode analytics to reduce spend in the newly announced BPCI Advanced Model by CMS.






